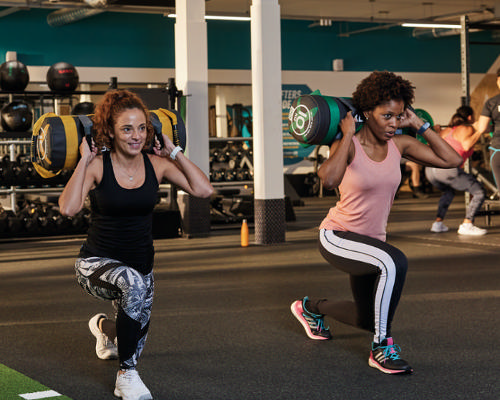Latest news
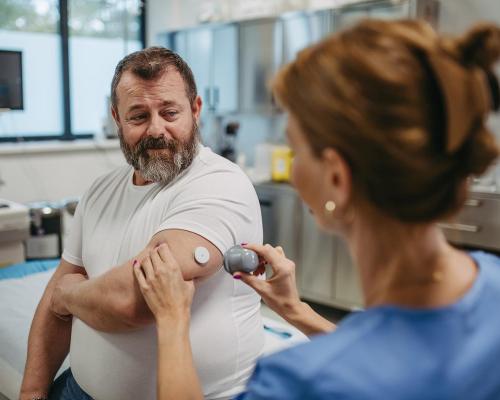
Paying men to lose weight could help fix obesity crisis
According to a year-long study, offering financial incentives to people to encourage them to lose weight is effective and could be a low-cost solution to support health service in tackling obesity.
Funded by the National Institute for Health Research in the UK, Game of Stones is a trial led by Professor Pat Hoddinott at the University of Stirling in Scotland, in association with five other universities. It has been published in The Journal of the American Medical Association and presented at the European Congress for Obesity in Venice.
A cohort of 585 men across Scotland, England and Northern Ireland were recruited and split into three groups. One group received daily supportive text messages, plus the opportunity to earn £400 for meeting weight loss goals. The second received only text messages and the third received no extra support or financial incentive.
The men were given targets of 5 per cent weight loss at three months, 10 per cent at six months and to maintain 10 per cent weight loss at 12 months – at which point the cash was paid.
Results were collated after one year and found the men receiving both text messages and offered cash lost the most weight, at 5 per cent. Those who received text messages lost 3 per cent of their body weight and the third group lost 1 per cent.
Hoddinott says men are a hard group to reach because they don’t like going to weight loss classes: “This was a carefully planned study, created for men by men. Various men’s health groups and charities were involved and more than 1,000 men living with obesity informed the design of the incentive structure.
“The research showed that offering cash incentives was a popular and effective way of helping men lose weight. This initiative would be a low-cost solution for the health service to offer men, requiring only four short weight appointments and with money paid out only at the end to those who lose over 5 per cent of their starting weight.”
With obesity and related diseases costing the UK's health services £6.5 billion annually, new approaches to tackling the problem are necessary. The researchers say this combination of financial reward and text messaging could be a low-cost solution.
Professor Katrina Turner, co-investigator from University of Bristol says: “We need effective weight loss interventions that can be implemented at scale and across different health settings. This is a low cost intervention with little impact on resources and a low burden for patients.”
The men who participated in the research had an average age of 51, with 39 per cent living in areas of lower socioeconomic status; 29 per cent reported a disability; 40 per cent had multiple long-term conditions and 25 per cent had been diagnosed with a mental health condition.
One successful participant said he liked the fact the initiative was aimed at men with specific targets and a competitive element. The financial incentive gave the project credibility with his peer group and made it seem more than a diet.
Another – who lost almost two stone – said the appointments were infrequent enough to be easy to attend, but regular enough to keep him accountable.